Sana Amir Akbar
Shaukat Khanum Memoral Cancer Hospital & Research Centre, Pakistan
Title: Primary hepatic neuroendocrine tumor – multimodal approach for diagnosis and management
Submitted Date: September 1 2017
Biography
Sana is a medical professional. Her educational background includes MBBS from Allama Iqbal Medical College, Lahore and one year of house job / internship from Jinnah Hospital, Lahore. She has recently cleared her intermediate module of residency training. Currently she is a working as a resident doctor in General Surgery at Shaukat Khanum Memoral Cancer Hospital & Research Centre, Lahore, Pakistan and is in third year of her FCPS-II training. Her area of interest includes Hepatobiliary surgeryrn
Abstract
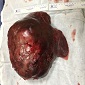
Background: Neuroendocrine tumors (NET) of the liver are generally metastatic lesions from other more common primary sites. Liver is an unusual primary site for a NET with only 150 reported cases in English literature. Here we present a case of a primary hepatic NET.Case presentation: A 64 years old gentleman with no known comorbids presented in outpatient department with 3 weeks history of pain in right upper abdomen associated with generalized weakness and poor appetite. Examination was unremarkable except for non tender hepatomegaly. CT scan liver showed a large 18.1 cm lesion in right lobe that was atypical for HCC.. Viral markers for Hepatitis B & C were non reactive. To confirm the diagnosis, biopsy of the lesion was performed that showed NET. Upper and lower GI endoscopies and whole body octreotide scan was performed to locate the primary lesion. These investigations revealed no lesion elsewhere in the body, so he was diagnosed with primary hepatic NET. It was managed with 1 cycle of neo adjuvant chemotherapy to reduce the size of the lesion followed by right portal venous embolization to increase the volume of future remnant liver. Right hepatic trisectionectomy was performed 1 month after PV embolization. Final histopatholgy showed 23 cm NET, WHO Grade-II with 2 mm nearest parenchymal margin.rnPost operative course was unremarkable and he was discharged on the 6th POD in stable condition. On his second follow-up visit, 8 weeks after surgery, he presented with right leg DVT and bilateral pulmonary embolism that was managed with therapeutic dose of enoxaparin and life long anticoagulation. Currently he is alive, disease free and on regular follow up.Conclusion: Primary hepatic NETs are challenging to diagnose but they can be successfully managed with multi modal treatment.

Renee Wong
St. George’s University School of Medicine, West Indies
Title: Unique case of retroperitoneal fibrosis masking a metastatic adenocarcinoma of unknown origin
Submitted Date: 11-08-2017
Biography
Renee Wong earned her Bachelor of Science with an Honor’s Specialization in Medical Sciences with Distinction from Western University, Canada, with participation in the Scholar’s Electives Research program. She is passionate about improving medicine through research and continually attaning and sharing knowledge. She is currently a 4th year medical student at St. Georgen’s University School of Medicine. Her recent publication includes a co-authored article “Nutrition Clinical Practice on Low Vitamin B12 in Patients in the Amputation Rehabilitation Unitâ€. She is a member of the American Academy of Family Physicians.
Abstract
Abstract\r\nRetroperitoneal fibrosis secondary to malignant disease is a rare condition associated with an ominous prognosis. We present the first reported case of retroperitoneal fibrosis related to metastatic adenocarcinoma of a primary occult tumor. This is a case of 64-year-old Caucasian male presented to the emergency department with his third episode of anuric acute renal failure despite bilateral ureteral stent placements and revision. A month earlier at first presentation with anuria, a CT scan revealed moderate bilateral hydronephrosis. He had an unprovoked DVT diagnosed 3 months prior. Examination demonstrated suprapubic tenderness and mild peripheral edema and no palpable lymphadenopathy. His creatinine was elevated at 5.42 and Hg low at 11.5mg/dL. CEA was elevated at 220.4, with normal CA 19-9, PSA and AFP. His IgG-4 (98mg/dL), LDH, ESR and CRP were elevated. Colonoscopy showed moderate diverticulosis of sigmoid colon with wall thickening. A F-18-FDG PET scan showed multifocal areas of metastatic malignancy in the neck, chest, abdomen, pelvis and bones. A liver biopsy showed infiltration by malignant epithelial cells in nests, consistent with gastrointestinal tract adenocarcinoma. Larger bilateral ureteral stents were placed and he was discharged 8 days later with normalised creatinine. Palliative outpatient chemotherapy was commenced. This case illustrates the importance of careful workup looking for an underlying cause of RF. Although malignancy is a relatively rare cause, its potential was highlighted by the unprovoked DVT, weight loss and smoking. The elevated CEA and subsequent PET scan led to a diagnostic biopsy. Recognition of this syndrome is critical in institution of appropriate therapy.
